One of the most important goals of Preventive Dentistry is to help patients maintain their teeth for life. When a tooth becomes compromised to the point that the pulp inside becomes inflamed or infected, root canal treatment may be the solution that allows us to save your tooth.
When Is Root Canal Treatment Needed?
The pulp is the innermost part of a tooth, containing nerve fibres and blood vessels. The tooth exterior usually protects it, but there are still many situations that can lead to the pulp becoming damaged, including:
- Deep decay that extends to the tooth interior
- Extensive dental work
- Tooth trauma or cracking
- Periodontal (gum) disease
- Extreme long-term wear and tear
Tooth Pulp Inflammation
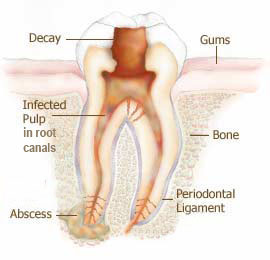 There are a few symptoms that might indicate the need for root canal treatment. One of the most common and distinct is painful sensitivity to both hot and cold, which often progresses into a constant, ongoing toothache. However, sometimes the tooth pulp can deteriorate without any signs at all.
There are a few symptoms that might indicate the need for root canal treatment. One of the most common and distinct is painful sensitivity to both hot and cold, which often progresses into a constant, ongoing toothache. However, sometimes the tooth pulp can deteriorate without any signs at all.
If pulpal inflammation doesn’t resolve and goes untreated, the tooth pulp will eventually die and usually becomes infected by oral bacteria. This infection follows the root canals down to the jawbone where it can cause infection and damage to the bone itself. At this stage, the tooth is usually very painful to touch and chew with. Left untreated, the pain will escalate, an abscess will form and the tooth will eventually need to be removed.
The Root Canal Treatment Process
Root canal treatment aims to remove the inflamed or infected pulp, disinfect the root canals, and then seal them so they won’t suffer from re-infection. After a root canal treatment, the pain resolves, the damaged bone heals and the tooth can be kept.
X-rays are taken during the procedure to determine the number, shape and precise length of canals. This is vital for ensuring that all canals are thoroughly disinfected.
Root canal treatment is usually performed over several appointments to allow time for anti-bacterial dressings to disinfect the canals. The use of local anaesthesia during treatment ensures that the procedure is comfortable.
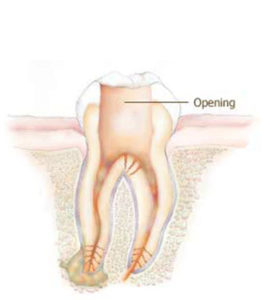
1. An opening is made through the top of the tooth into the chamber where the pulp is found.
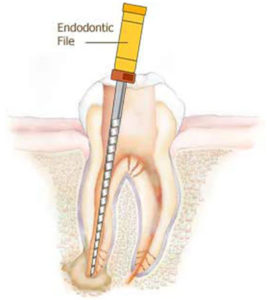
2. The pulp is removed, and the root canal/s are cleaned and shaped using endodontic files. Anti-bacterial dressing is placed and remains in the canals between appointments. The opening is sealed with a temporary filling. Sometimes the tooth will need to be dressed more than once – this depends on the severity of the infection.
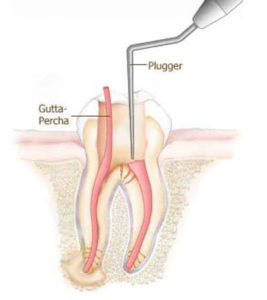
3. At a subsequent appointment, the temporary filling will be removed, and after cleaning, the root canal/s will be filled with a material called gutta-percha.
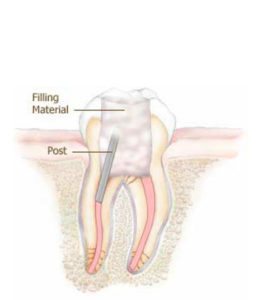
4. Finally, a core filling is placed to seal the opening in the tooth. The tooth is now ready to receive a crown.
Endodontist Referral
An Endodontist is a specialist in root canal treatment. Difficult cases may require referral to an Endodontist to achieve the best possible outcome.
Crown Placement
Clinical research has shown that root canal treated teeth are structurally weaker and therefore more prone to fracture. This is especially true of back teeth that receive heavy forces. Hence, a crown is often recommended for such teeth to restore their function and help protect against breakage.
Contact Preventive Dentistry for more information about root canal treatment or to arrange an appointment.